Health Strategy.
Somatic mutations of DNA genes are still considered the main factor in the occurrence of cancer. However, modification of nuclear DNA is only a part of the overall picture of the tumor process, and not its main cause. Even multiple mutations in nuclear DNA do not provide the cell with the inevitable cancerous characteristics.
Several studies have shown that when the nucleus of a cancer cell was combined with the contents of a normal cell, signs of malignancy did not appear * * * * *. Even in the presence of tumor-associated mutations, the carcinogenicity of many types of tumors was suppressed when the tumor cell nucleus was introduced into the cytoplasm of a normal cell * * * *. Conversely, carcinogenicity increased when the contents of a cancer cell were combined with the nucleus of a normal cell * *.
But this was about the fusion of material, but what if we try to cross-transplant the nuclei of normal and cancer cells? Such experiments have also been carried out. When the nucleus in a cancer cell was replaced with that of a healthy cell, it continued to show malignancy. And when in a healthy cell the nucleus was replaced by the nucleus of a cancer cell, it continued to show non-malignant * *.
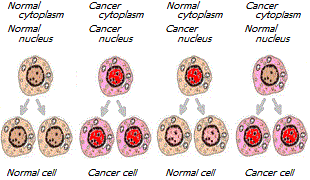
The nuclei of cancer cells after their transplantation into a healthy cytoplasm formed normal tissues *. From cancer cells introduced into early embryos, healthy tissues and organs were formed *. After the introduction of the nucleus of a cancerous frog cell into an ovum with a healthy nucleus previously removed from it, the ovum developed into a healthy tadpole *. If, as it is stubbornly asserted, nuclear DNA gene mutations were indeed the only, or even the main, cause of cancer, such miracles would not be possible. The malignant characteristics would have to be carried along with the nucleus of the malignant cell.
Intrigued by these discoveries, researchers conducted similar experiments with mitochondrial transfer. When mitochondria of a normal cell were added inside a tumor cell, the oncogenic phenotype of the latter was suppressed * * *, and its sensitivity to chemotherapy was aggravated *. At the same time, when mitochondria of a tumor cell were added inside a normal cell, the oncogenic phenotype of the latter was enhanced * *. Thus, the degree of malignancy of a cell is dictated by the state of its mitochondria and, possibly, other cell organelles.
Indeed, intracellular factors can suppress the tumor phenotype * or, conversely, stimulate it. Mutations in mitochondrial DNA or other factors can disrupt the oxidative phosphorylation process *, forcing the cell to turn to glycolytic energy production. In addition, persistent pathogenic mutations in mtDNA can also lead to epigenetic changes that cause genomic instability in the nuclear genome.
The most reasonable explanation for the results of the experiments listed above is that for malignant transformation of cells, genetic changes in nuclear DNA are insufficient, if at all necessary. It seems that the malignant transformation of cells is the result of defects in the cytoplasm, and not defects in the nucleus *. When mitochondria function normally, then carcinogenic mutations in nuclear DNA have little chance of being realized. Healthy mitochondria can reverse the cancerous behavior of cells even with mutated nuclear DNA, and vice versa, mitochondrial dysfunction will force cells to increase glycolysis and fermentation, inducing cells with normal DNA to malignant transformation.
The tumor phenotype can be returned to the normal phenotype not only at the cellular level. The state of the tissue and, by and large, the whole organism is decisive in the question of whether a tumor will form or not, and what will be its fate. Tissue with fully differentiated cells is able to successfully influence the behavior of emerging malignant cells towards their correction.
Transplantation of cancer cells into healthy tissue can lead to the loss of their malignant properties, despite the presence of mutations * *. Not only a single cancer cell, but even a sufficiently large group of cancer cells have no chance of forming a tumor if the tissue into which they are implanted is healthy. In order for a human to form a tumor, a simultaneous injection of at least 10 million cancer cells * is required. When too few cancer cells are introduced from a tumor into healthy tissue, they completely lose their malignancy and turn into normal cells * *, although this should not be the case with irreversible genome defects.
Finally, cancer cells, under certain microenvironmental conditions, are able not only to stop their growth, but also to turn to a normal phenotype * *. Such cases are called spontaneous remission. All of these facts somehow do not agree well with the prevailing theory that cancer comes from a single mutated cell that has lost control, and that its development is irreversible.
The ever-growing body of evidence strongly suggests that the current view of the origin and nature of cancer needs to be revised. That the tumor is more of a metabolic than a genetic disease *. And that the mitochondrial metabolic theory (MMT) can better explain the signs of cancer than the somatic mutation theory (SMT) *.
From the point of view of metabolism, it is the pathological violation of cellular respiration that is the center of the problem. It is it that precedes *, and is the cause of the instability of the genome, which accompanies the process of tumor development. While short-term genomic instability may not be sufficient for genetic mutations, long-term instability increases this risk. Among the nuclear DNA mutations that have arisen, there may be those that contribute to further metabolic disorders, malignant transformations, and disease progression.
Targeting an anti-cancer strategy at a genetic problem, which guides modern medicine, does not make practical sense. In decades of research, no single specific causative gene or set of genes has been identified for the vast majority of cancers. Mutations in cancer cells occur in millions of unpredictable places in DNA, giving each case its own personality. And, in terms of genetics, each of them may require individual treatment. Meanwhile, tumor cells will acquire more and more new mutations. Finally, cancer cells can exist without any mutation at all.
At the same time, the mitochondrial problem is common to almost any case of cancer. Cells with poorly functioning mitochondria may not be cancerous. However, it is unlikely that there will be cancer cells with fully functional mitochondria. From it point of view, the treatment of most cases of cancer can be reduced to a common protocol.
If the defect in tumor cells really lies in the mitochondria, and not in the cell nucleus, then this completely changes the approach to cancer treatment. Instead of, or at the same time, focusing on the destruction of cells with irreversibly mutated genes, one should focus on restoring the normal functioning of mitochondria in all cells of the body.
Living mechanisms have an inherent desire for organization, orderliness and development, while non-living mechanisms have an inherent desire for chaos, disorder and destruction. The chemistry of living nature differs from the chemistry of inanimate nature in that the processes in it proceed in a controlled manner, with the help of appropriate enzymes and the coordinated work of electrochemical mechanisms. However, the control of biochemical reactions requires energy costs, so no living organism can exist without energy supply.
The main part of the energy produced by human cells is extracted from glucose molecules. First, glucose is transported into the cell and participates in a process called glycolysis. This is a multi-stage biochemical process that takes place in the cytosol of the cell. Each of the ten metabolic reactions of glycolysis requires specific enzymes and does not require oxygen. Glycolysis does not break down the glucose molecule to the end, and therefore does not release all the energy available in it.
As a result of glycolysis, 2 molecules of pyruvate (pyruvic acid) are formed from 1 molecule of glucose and 2 molecules of adenosine triphosphate (ATP) are charged with energy, which is used by all cells of the body as an energy agent. The resulting pyruvate from glycolysis can then be metabolized to lactate and excreted from the cell as metabolic waste. Most primitive life forms produce energy in this way, and they did it long before oxygen appeared in the atmosphere of the planet (about 2.5 billion years ago). Such unicellular organisms also have such characteristics of cancer cells as uncontrolled division and immortality.
Cells of highly organized organisms have the ability to break down pyruvate further, forming only water and carbon dioxide as metabolic waste products. This is done in cellular organelles called mitochondria, first in a cyclic biochemical process called the Krebs cycle (KC) and then in an electrochemical process called oxidative phosphorylation (OP). In such cells, from each glucose molecule, 2 ATP molecules can be produced, as before, using glycolysis, and up to 36 additional ATP molecules using OP. The latter process requires the consumption of oxygen, which serves here as an electron acceptor in the final stage of energy production – the so-called «electron transport chains».
In human cells, more than 90% of intracellular ATP is produced precisely by OP *. Despite the fact that OP needs an oxygen supply, this mode of energy production is many times more efficient than glycolysis. Surprisingly, some cells in the human body continue to use glycolysis as their main source of energy (eg, erythrocytes, retinal cells, testis cells). These are normal glycolytic cells. However, all other normal cells, including epithelial cells, use OP as the main energy generator.
Impaired cellular energy metabolism is a defining characteristic in almost all cancers. If in normal epithelial cells the vast majority of all energy is produced by mitochondria, then in cancer cells, mitochondria largely lose their function. This not only radically changes the picture of energy metabolism. During the various stages of glycolysis, chemical raw materials are formed as metabolic waste products, which make it possible to build a daughter cancer cell from it. The more intense glycolysis, the more such building material, the faster the cancer cell can divide.
So, in most cases, cancer cells are characterized by increased glycolysis – the conversion of glucose into pyruvate and further increased metabolism of the resulting pyruvate into lactate. Many normal cells during hypoxia can also temporarily increase enzymatic energy production, but when adequate oxygen levels are restored, they always return to mitochondrial energy production. Cancer cells do not, however, use glycolysis even in the presence of sufficient oxygen (a phenomenon called aerobic glycolysis).
The increase in energy production through fermentation is not only a consequence of the previous stages of the development of the tumor process, but also the cause of its subsequent stages. Long-term dependence of cells on enzymatic energy production exhibits cancerous cell characteristics such as genomic instability, intracellular metabolic disturbance *, acid-base reversal *, loss of differentiation, and uncontrolled growth *. Thus, enhancement of mitochondrial respiration of cells has an important therapeutic value * *.
The restoration of natural cellular metabolism includes two complementary actions: the weakening of anaerobic respiration and the strengthening of aerobic respiration.
Mitochondrial support. Mitochondria are active cellular organelles, the number of which in each cell can vary from 200 to 2'000. They have their own DNA, which they use for their reproduction, and are a kind of intracellular symbiont cohabitant. Presumably, mitochondria originated from free-living bacteria that used the OP mechanism to produce their energy.
It is believed that several hundred million years ago they were taken up by an ancient glycolytic host cell, but were not internalized and were instead incorporated into its intracellular processes, providing the cell with significant evolutionary advantages. Further, this symbiont cell became the progenitor of all living organisms whose cells use OP.
The main cellular function of mitochondria is the production of energy necessary for the metabolic processes of the cell. The energy source for the cells of the human body can be various nutrients, but ultimately this energy is stored only in a molecule called adenosine triphosphate (ATP). ATP is used for energy by all cells, both healthy and cancerous.
Mitochondria not only produce energy, but also take part in a number of other extremely important cellular functions. This is the regulation of membrane potential and differentiation; cell signaling through reactive oxygen species (ROS); calcium signaling, control of apoptosis and autophagy; regulation of cellular metabolism; regulation of iron metabolism and heme synthesis; regulation of steroid synthesis *. Thus, the health of the cell and the whole organism depends on the health of mitochondria.
Mitochondria undergo specific structural and functional changes in cancer, and they are actively involved in metabolic reprogramming. A decrease in the number of mitochondria and/or their functionality is considered a characteristic feature of cancer cells. Of course, loss of mitochondrial function is not always associated with malignant transformation; other conditions are required for such a switch, but malignant transformations are almost always associated with loss of mitochondrial functions.
In the process of ATP production in mitochondria, a large number of free radicals (oxidants) appear, such as reactive oxygen species (ROS) and reactive nitrogen species (APA). The more raw materials for energy enter the mitochondria, and the more actively it is produced, the more free radicals are formed, the stronger their destructive effect. And it is not so important whether energy is produced from glucose, lipids or amino acids, their total amount is important.
The resulting free radicals damage any proteins, primarily the mitochondria itself, which leads to degradation of the inner layer of its membrane and disruption of the process of oxidative phosphorylation. Therefore, even with a large amount of incoming raw materials, energy production through the OP can fall. The unprocessed excess of raw materials accumulates in the cell, clogging its internal space. Oxidative stress in mitochondria also causes instability of the mitochondrial and even nuclear genome and enhances the expression of oncogenes. In addition, high levels of oxidants trigger a cascade of events that decrease proteasome activity, decrease telomere length, and impair immune function.
Since the formation of free radicals is as natural in the process of energy production as the formation of smoke when burning wood, natural defense mechanisms are provided in the cell to neutralize them. This is, first of all, glutathione, which is the most powerful intracellular antioxidant. Insufficient production of glutathione, or its depletion due to a large number of oxidants, or both, will lead to the degradation of OP.
In addition to oxidative damage, mitochondria can experience other aggressive attacks that lead to a weakening of the RP process, and to a further increase in the level of free radicals and other mitochondrial toxins. This further exacerbates the situation, dispersing the destructive vicious circle *. At the same time, mitochondrial functions, including the production of ATP, are naturally suppressed, which entails the most serious consequences.
Mitochondrial toxicity can be induced by some drugs, through various mechanisms such as mitochondrial DNA depletion (eg, nucleoside reverse transcriptase inhibitors), inhibition of fatty acid beta-oxidation (eg, valproic acid), opening of mitochondrial permeability transition pores (eg, anthracyclines), creation of oxidative stress and mitochondrial glutathione depletion (eg, acetaminophen), uncoupling of electron transport from ATP synthesis (eg, tamoxifen), and inhibition of mitochondrial electron transport chain complexes (eg, statins) *.
A significant part of the energy produced by mitochondria is spent on the work of ion pumps built into the cell membrane *, which maintain a balance between intracellular ions (potassium and magnesium) and extracellular ions (calcium and sodium). The quantitative difference between sodium and potassium ions on both sides of the cell membrane creates a certain electrical potential on it, which supports many cellular functions.
Due to the lack of energy, the efficiency of sodium-potassium membrane pumps decreases. The intracellular level of sodium ions relative to potassium ions increases, which negatively affects the function of cell membranes. Due to the imbalance of sodium and potassium ions, the electrical potential on the membrane of the transforming cell decreases, creating an increasingly negative field around it. This worsens the functional state of the cell. In addition, such a cell acquires the ability to repel negatively charged drugs and cells such as red blood cells and lymphocytes, preventing oxygen and the immune system from counteracting the tumor.
Another part of the cell's energy is spent on the synthesis of enzymes, thanks to which the chemical reactions inside the cell become controlled. The lack of certain enzymes further impairs CK and RP. When the supply of glucose and other sources of energy to the cell is sufficient, but the mitochondria are not able to provide the necessary level of energy, the cell is forced to turn to an older and less profitable principle of energy production, increasing glycolysis and fermentation *. And this is one of the first steps of the malignant degeneration of the cell.
A deep energy deficit forces the production of only those enzymes that are needed only for the survival of the cell. With a decrease in energy supply, such cellular functions of mitochondria as differentiation, inhibition of cell growth, and apoptosis deteriorate. Through apoptosis, abnormal cells are removed, thereby preventing the cancer process. If apoptosis does not work well, then such cells can remain alive and reproduce offspring with the same defective mitochondria.
In addition, the cell of a multicellular organism must coordinate its behavior with other cells. She does this by capturing the slightest nuances of the concentration of chemical signals and electric fields. The operation of such sensory mechanisms also requires energy consumption. The stronger the energy deficit in the cell, the worse the communication of the cell, the less it responds to social demands, the weaker it responds to the signals restraining unbridled growth, the deeper it plunges into the selfish behavior of its single-celled ancestor, the more it acquires cancerous signs.
Both poorly functioning mitochondria and a small number of them contribute to switching the cell phenotype to a malignant one. In cancer cells, there may actually be an increase in the number of mitochondria in order to compensate for the loss of their functions in this way *. However, such efforts are not capable of fundamentally solving the energy problem until its fundamental causes are eliminated. Without this, mitochondria, even with a large number of them, will remain defective.
Thus, long-term dysfunction of mitochondria, manifested as a lack of oxidative phosphorylation, in combination with increased glycolysis and glutaminolysis, can lead the cell to enter a steady state of unrestrained proliferation – with further loss of differentiation, with resistance to apoptosis, and with other characteristic features signs of a cancer cell. Moreover, emerging evidence indicates that mitochondrial changes contribute not only to malignant cell transformation, but also to angiogenetic, invasive, and metastatic behavior of cancer cells *.
Mitochondrial dysfunction is a telling signal of aging and a feature of virtually all degenerative diseases *, not just cancer * *. More and more deteriorating work of mitochondria as the years go by is observed not only in humans, but also in other animals. However, we can improve mitochondrial health to some extent. Mitochondrial respiration can be enhanced in several ways, such as by reducing oxidative stress; an increase in the number of mitochondria; normalization of their metabolism; the ability to replace defective components; mitophagy and apoptosis *.
Certain supplements * * may help improve mitochondrial function. They are able to reduce oxidative load, provide additional opportunities for oxidative phosphorylation, strengthen leaky mitochondrial membranes, and remove non-functional mitochondria.
Cofactors and antioxidants:
• Coenzyme Q10 (CoQ10) is involved in the mitochondrial production of ATP, in fact, at the stage of OP. CoQ10 supplementation increases mitochondrial cellular energy production, as well as the number and activity of macrophages and T-lymphocytes *, and the level of immunoglobulin G (GIg) antibodies * * *.
The best is considered CoQ10 of the Japanese company «Kaneka», which is extracted from mushrooms. Foods rich in CoQ10 include salmon, organ meats, whole grains, peanuts, pistachios, walnuts, hazelnuts, sesame seeds, soybeans, olive oil, avocados, broccoli, and spinach.
In combination with creatine (2×3'000mg) and lipoic acid (2×300mg), CoQ10 (2×120mg) increases mitochondrial ATP production in patients and reduces plasma lactate concentration *. In this combination, CoQ10 enhances the function of the electron transport chain, lipoic acid acts as an antioxidant, and creatine acts as an energy buffer.
Another CoQ10 booster could be shilajit (200 mg/day), which allows it to retain its antioxidant properties longer *.
Endogenous CoQ10 levels decline with age, so exogenous CoQ10 supplementation could improve mitochondrial function and increase mitochondrial complex I activity in the electron transport chain. Dosage of shilajit: 3×100 mg for prevention and 3×200 mg during the course of treatment *.
• Nicotinamide riboside is a form of vitamin B3, a metabolic precursor of NAD+ that is a cofactor in over 200 cellular redox reactions, including mitochondrial ATP production. By improving the function of mitochondria, aging stem cells of various tissues become more youthful with an increase in the level of NAD+ in cells * *.
Higher levels of NAD+ in cells correlate with improved health outcomes *, and vice versa, lower levels of NAD+ contribute to the development of many degenerative diseases *. With age, the concentration of NAD+ gradually decreases: by the age of 50 – by 40%, and by 80 years – by 90-95% compared to the age of 21 *. However, nicotinamide riboside supplementation (2×500 mg/day) rapidly restores blood NAD+ levels to younger levels. Compared with the placebo group, nicotinamide riboside at 300 mg/day increased cellular NAD+ levels by 51% in older adults and also increased glutathione and reduced fatigue *.
Since NAD+ is an endogenous substance, supplementing it in old age actually means bringing NAD+ levels to the level corresponding to a young age. While CoQ10, by adding energy, can simultaneously increase the number of free radicals in mitochondria, nicotinamide, on the contrary, reduces their number *. It can be assumed that a combination of both will have a better effect than CoQ10 alone.
• N-acetylcysteine (NAC) is a precursor of glutathione. It increases the activity of mitochondrial complexes I, IV and V; strengthens the mitochondrial membrane and improves mitochondrial homeostasis *. Dosage: 250-1'800 mg/day * *, (usually 600 mg/day). N-acetylcysteine is poorly absorbed, so it is recommended to take its liposomal form (2×250 mg) or S-acetylglutathione (2×100 mg).
The use of glutathione precursors is better than using glutathione directly (inhaled or intravenously). In the first case, the body produces exactly as much glutathione as it needs. In the second case, glutathione can be either too little or too much.
The combination of NAC with glycine allows you to increase the concentration of glutathione inside the mitochondria, and fill the cells with younger and more efficient mitochondria. At the same time, oxidative stress and inflammation indicators are reduced, and the metabolism of fats in the cell improves. This has been convincingly proven in a classic 16-week, double-blind, randomized clinical trial *. Here, the daily dosage of NAC and glycine was 100 mg each per 1 kg of patient weight; those 6 grams each with a weight of 60 kg, which is twice the daily requirement of glycine. Interestingly, the positive effects of the supplements were seen only in the elderly, but not in younger people.
• Alpha Lipoic Acid (ALA) is a powerful antioxidant and also a chelator of metal ions such as copper and iron. It acts as a critical cofactor for mitochondrial processes and increases the levels of the mitochondrial antioxidants glutathione and vitamin C.
Consumption of alpha-lipoic acid (2×500 mg) increases mitochondrial membrane potential and also protects DNA and cell membranes from exercise-induced oxidative stress *.
• Melatonin (3 mg at bedtime, but not more than 15 mg) is a broad-spectrum non-steroidal hormone that effectively protects mitochondrial function *.
Melatonin promotes the switch from glycolytic to mitochondrial cellular energy production. In one clinical study, melatonin effectively counteracted the oxidative stress and mitochondrial dysfunction that was caused by sepsis *.
However, melatonin is best taken only for sleep problems, and its beneficial effect on mitochondria will be received as an additional bonus.
Vitamins and minerals:
• Pyrroloquinoline quinone (PQQ), also known as methoxanthin (vitamin B14), protects mitochondria from oxidative damage *,
increases the efficiency of mitochondria due to their rejuvenation and increased activity * * *.
In addition, methoxanthin raises hemoglobin levels and reduces plasma concentrations of inflammatory markers such as IL-6 and CRP *.
The addition of methoxanthine to the diet of animals increases the number of mitochondria in their cells * *.
Methoxanthin 20 mg/day for 12 weeks helps prevent decline in brain function in the elderly, especially with regard to attention and working memory *,
and also reduces LDL blood levels compared to controls *.
Dosage: 15-25 mg/day *.
PQQ does not cause acute toxicity at dosages up to 60 mg/day.
• Vitamin C (3×300 mg) *; vitamin E; B group vitamins * – thiamine (100 mg/day) * *, riboflavin (100 mg/day) *, niacin (50 mg/day), pantothenic acid (50 mg/day), biotin (30 μg/day); and magnesium citrate (2-3×500 mg) *; mixed phospholipids (1-2×1'000 mg) * *; succinic acid (125 mg/day); ginkgo biloba (40 mg/day); succinate (125 mg/day) may also improve mitochondrial function in various ways *.
However, this apparently applies to those cases where their intake with food is not enough.
Mixtures of various of these antioxidants will apparently be more effective than either of them alone *.
However, there are still too few clinical studies evaluating their combinations * * *.
Although vitamin and mineral supplements are usually beneficial only when they are deficient, this condition is more commonly seen in cancer patients.
• Calcium and magnesium are essential for mitochondrial energy production, so make sure you get enough of them in your diet.
• Lithium has improved mitochondrial function in preclinical studies * *. However, evidence for its benefit in cancer has not yet been provided.
Lipids and transporters:
• Omega-3 fatty acids (3×1'000 mg) help maintain the integrity of the mitochondrial membrane and repair it in the event of oxidative damage.
• Medium chain fatty acids (MCFAs) provide better mitochondrial respiration capacity than long chain fatty acids without increasing oxidative stress *.
• L-carnitine helps the passage of fatty acids through the inner mitochondrial membrane. It promotes increased energy production from fatty acids, protects mitochondria from oxidative stress, and increases the rate of oxidative phosphorylation in mitochondria *.
Clinical studies show an increase in the functionality of mitochondria due to the intake of 1-2 g/day of L-carnitine * * *,
(usually 3×500 mg).
• Acetyl-L-carnitine is a more effective version of L-carnitine. It acts synergistically with alpha lipoic acid to rejuvenate decrepit mitochondria. Dosage: 300-3'000 mg/day, (usually 3×250 mg).
Mitochondrial modulators:
• Metformin is actually a mitochondrial toxin. It worsens the work of the OP, which, it would seem, contradicts what we need. However, the reduction in energy production produces a culling of the weakest mitochondria, essentially just finishing them off. This process is called mitophagy. It is assumed that destroyed mitochondria are subsequently replaced by younger and better ones. Thanks to this, energy production through OP increases, and the negative impact of non-functional mitochondria decreases.
Thus, at the maximum dose allowed for diabetes (36 mg/kg), metformin helps improve the quality of mitochondria in the cell *. Substances with similar properties that help improve the functioning of the mitochondria of cancer cells are called mitocanes (an abbreviation for the words mitochondria and cancer).
Another explanation for the paradox of why mitochondrial toxins have the opposite effect is the theory of hormesis. According to this concept, low doses of toxines trigger beneficial compensatory responses that surpass the repair of the triggering damage and actually produce an improvement in cellular fitness when compared to the starting predamage conditions.
In premenopausal patients receiving long-term metformin (1'500 mg/day for 16 weeks), mitochondria showed an increase in oxygen consumption, an increase in membrane potential, mitochondrial mass, and a decrease in free radical concentration compared to control *. Dosage: up to 1'500 mg/day *.
In addition, through other mechanisms, metformin mimics some of the biological benefits of calorie restriction (improved exercise performance, improved insulin sensitivity, reduced LDL and cholesterol levels) without actually reducing caloric intake.
As you can see, metformin acts in a direction that is opposite to other mitochondrial modulators. For example, CoQ10 is an active player in the electron transport chain, while metformin blocks the operation of the electron transport chain. A fair question arises, is it possible to combine metformin, for example, with the coenzyme CoQ10? Some animal studies suggest that CoQ10 and metformin do not interfere with each other * *. It seems that while metformin removes cells with weak mitochondria, CoQ10 strengthens cells with more or less functional mitochondria. However, the question remains open.
• Urolithin A, like metformin, promotes the death of dysfunctional mitochondria. The action of both of these substances can be compared with the action of predators in wildlife, which paradoxically promote the survival of the biological species of their victims by deleting the weakest individuals.
A systematic review including a total of 41 animal studies noted the neuroprotective, antimetabolic activity, as well as nephroprotective, myocardial, anti-inflammatory and musculoskeletal protection of urolithin A, urolithin B and a synthetic analogue of methylated urolithin A *.
A controlled 4-month clinical trial showed that urolithin A (Mitopure™) supplementation of 500-1'000 mg/day in older adults (40-64 years) slightly improved mitochondrial function. This was reflected in increased muscle strength, performance and peak oxygen consumption. In addition, urolithin A reduced levels of inflammatory markers such as C-reactive protein *. Another 4-month controlled clinical trial in older adults (65-90 years old) showed similar results. Taking 1'000 mg/day of urolithin A compared to placebo increased muscle endurance and decreased C-reactive protein levels, although these changes were not significant *.
In the human body, urolithin A is naturally produced from ellagic acid and its derivatives with the help of intestinal bacteria. Rich sources of urolithin A precursors include foods such as pomegranate, strawberries, walnuts, raspberries and almonds. However, not all intestinal bacteria contribute to the production of urolithin. One study found that people with a higher Firmicutes:Bacteroidetes ratio (where a low ratio has been associated with gut dysbiosis) and more Clostridiales, Ruminococcaceae and Akkermansia muciniphilia are better producers of urolithin A *.
A huge part of the population experiences a deterioration in the ratio of Firmicutes bacteria to its antagonistic phyla of bacteria (Bacteroidetes) in favor of the latter. Normalizing the balance between these two groups of bacteria would undoubtedly bring significant benefits. However, from a practical point of view, it is difficult to correct the intestinal microflora, just as it is difficult to control the results of this correction. Thus, urolithin A supplements seem to be a more reliable and effective way to increase its concentration in the body.
• Betaine, also known as trimethylglycine, which is rich in table red beets, in vitro stimulates an increase in the number and activity of mitochondria *, and leads to an increase in mitochondrial respiration *.
Combinations of some of the above agents have been clinically tested. In one two-month study, patients with intractable chronic fatigue improved fatigue scores by a third when taking membrane phospholipids (2'000 mg/day), CoQ10 (35 mg/day), microencapsulated NADH (35 mg/day), L-carnitine (160 mg/day), α-ketoglutaric acid (180 mg/day), as well as lipids and other additives * *.
Physical activity. Mitochondrial functionality can be improved and maintained by stimulating autophagy, as well as by reducing calorie intake and moderate physical activity * *.Indeed, an increase in physical activity leads to increased autophagy * * and an increase in energy levels, which means more efficient functioning of mitochondria. This stimulates cells to increase the number and quality of mitochondria.
Additionally, stress-reducing practices such as meditation or yoga, as well as adequate sleep, may be helpful. A healthy diet, detoxification, and reduced inflammation and associated oxidative stress also protect mitochondria from chemical damage that reduces mitochondrial DNA copy number and ATP production. Techniques for reducing inflammation levels will be discussed in the «Anti-inflammatory therapy» section †.
Emotional condition. It seems incredible, but one study reported an association between positive emotions and the ability of mitochondria to produce energy *. Increased positive mood increased the enzymatic activity of the mitochondrial respiratory chain, as well as the number of copies of mitochondrial DNA. People's psychological state in the 3 days before blood was drawn predicted their mitochondrial health index, but not vice versa, suggesting a cause-and-effect relationship.
In this case, the mitochondria of immune cells (leukocytes) were studied, which may be directly related to their ability to destroy pathogens. But, as one might assume, the mitochondrial health of other cells in the body can also depend on a person’s emotional mood through a complex system of hormonal and other cellular communication.
Restriction of energy resources. The mitochondria of cancer cells are unable to produce sufficient levels of energy due to structural and/or functional abnormalities *. And although cancer cells significantly increase energy production through glycolysis, mitochondrial energy production is still critical for them. A further decrease in the energy of cancer cells can lead to their death, and the tumor – to a decrease in the growth rate.
The results of more than 30 years of research convincingly prove that calorie restriction is probably the most powerful and widely used nutritional intervention to suppress the process of carcinogenesis *. Metabolic nutrient overload causes defragmentation of the cell's mitochondrial network, while intermittent fasting induces autophagy, which removes dysfunctional mitochondria.
It can be reasonably assumed that excess calories and lack of oxygen significantly weaken the inhibition of cell proliferation and accelerate the formation of a cancerous cell phenotype. On the other hand, a lack of calories and sufficient oxygen inhibits cell growth and stimulates autophagy, which removes poorly functional organelles and cells, including cancer cells.
Indeed, theoretical models show that increased tissue fueling leads to rapid onset of cancer cell hallmarks such as rampant growth and tissue invasion *. If in the absence of glucose the competitive advantage is on the side of the cells with more economical aerobic respiration, then in the case of an abundance of glucose it is on the side of the cells with faster anaerobic respiration *.
In other words, unlimited resource conditions promote the spread of the cancer phenotype, while limited resource conditions prevent it. Based on this fundamental position, energy hunger should not only reduce the risk of cancer, but also contribute to the suppression of cancer cells and incline them to mitochondrial respiration.
Indeed, limiting the supply of raw materials for energy production to cells significantly slows the growth and development of many types of cancer, including breast cancer *. This reduces not only the level of insulin, but also the level of growth factor IGF-1, which stimulates the metabolism and growth of tumor cells *. While any therapeutic agent targets one or more targets, cellular energy restriction covers a range of therapeutic targets, including inflammation and angiogenesis * *.
We can limit the energy resources of cells using the following methods:
Reducing the volume and calorie content of food. Caloric restriction can cause the suppression of many of the genes and metabolic pathways that regulate glycolysis *. The Physiological Minimum recommended by The Office of Disease Prevention and Health Promotion for women of average build is ~ 1'600 kcal/day *, however, this value should be adjusted depending on age, height, index body weight and level of physical activity *. At a given minimum level, the maximum daily caloric intake should not exceed 2'400 kcal/day. It is this range of daily calorie values that is associated with the lowest morbidity rates *.
However, even a low-calorie diet should be adequate. If the food cannot provide sufficient levels of essential substances, they will have to be taken in the form of supplements. This is especially true for riboflavin, nicotinamide, pantothenic acid, other vitamins and enzymes involved in michondrial function.
Since fats have the highest calorie content, and carbohydrates have the least, it is easiest to reduce calories consumed at the expense of fat.
Decreased intake of carbohydrates in the body. There are several weight loss drugs based on the principle of reducing the absorption of carbohydrates from food.
The most famous and studied of them is metformin. Other natural glucose uptake inhibitors such as resveratrol, fisetin, myricetin, quercetin, apigenin, cyanidin, daidzein, hesperetin, naringenin, catechin *, genistein *, and silibinin * have shown similar effects in preclinical studies. However, their effectiveness compared to metformin is quite low.
Gluconeogenesis inhibition (inhibition of glucose production in the liver).
The most affordable, tested and safe drug that reduces gluconeogenesis is the same metformin.
Depletion of blood glucose levels due to its increased consumption. Muscle cells use glucose as their main energy source, while brain neurons use it as their sole source of energy. An increase in physical and mental activity will thus increase the consumption of glucose and reduce the level of insulin in the blood. In turn, consistently low glucose and insulin levels will help maintain optimal mitochondrial health.
It has been noted that under conditions of hypoxia, mammary gland cells accumulate a large supply of energy in the form of glycogen, which contributes to the protection of cells from oxidants and proliferation. Moreover, the more aggressive the tumor, the more glycogen accumulates in it *. The specific glycogen stores in an aggressive tumor can be comparable to those in the liver. Disabling the ability to use this energy with glycogen phosphorylase (an inhibitor of the enzyme responsible for breaking down glycogen) makes cancerous cells much less aggressive *. It is noteworthy that only the isoform of the enzyme that is characteristic of the brain, and not the liver, is effective here. Despite the temptation of such a proposal, its clinical application is still very far away.
Limiting the entry of glucose into the cell. Glucose is transported into cells by either the passive membrane transporters GLUT or the ATP-dependent and sodium-dependent transporter SGLT. By paralyzing the work of these transporters, it is possible to reduce the flow of glucose into the cell. Several herbal remedies are known to be able to moderately inhibit glucose transporters in vitro.
These are catechin, daidzein, hesperetin, fisetin, naringenin * and other flavonoids. The modes of action of natural inhibitors can, however, vary markedly.
Genistein, for example, binds the GLUT1 transporter on the outer surface, while quercetin interacts with its inner surface *.
Quercetin and EGCG *, luteolin, kaempferol *, silibinin, theaflavin inhibit insulin-stimulated glucose uptake.
It seems that their combination will be more effective than each of the inhibitors alone.
It would be logical to limit the flow of glucose into cells. But under the condition of a high concentration of glucose in the blood, insulin will strongly protest against such a decision. Because its job is to lower the blood glucose by pushing it into the cells. If we can make it difficult for glucose to be imported into the cells, both glucose and insulin levels in the blood can be high. That is, we will create the symptoms of type II diabetes. This means that it is possible to resort to limiting the entry of glucose into the cell only if its concentration in the blood is within safe limits.
Suppression of the process of glycolysis in cells reduces the amount of raw materials for energy production. As already mentioned, a lack of pyruvate will slow down the division of cancer cells, and a serious deficiency of it will cause cell death.
Currently, a limited number of specially designed glycolysis inhibitors are used, and all of them have certain disadvantages.
• Imatinib is a tyrosine kinase inhibitor. It inhibits the activity of the first enzyme of the metabolic chain of glycolysis – hexokinase, and this blocks all other enzymatic conversions of glucose into pyruvate. In addition, imatinib inhibits platelet growth factor (PDGF) and stem cell factor (SCF) receptor activity. Approved for clinical use in leukemia. The inhibition of hexokinase, in comparison with the inhibition of other glycolysis enzymes, is more beneficial because hexokinase can block cell apoptosis.
Lonidamine * also inhibits hexokinase.
• 3-bromopyruvate (3-BrPA) is a clinically used drug that inhibits hexokinase activity. To date, it is the most powerful of the clinically used means of inhibiting anaerobic respiration. Bromopyruvate inhibits respiration more actively in cancer cells, because there are much fewer transporters in normal cells that can move 3-BrPA into cells.
• Clotrimazole, used in antifungal therapy, in vitro displaces hexokinase from the mitochondrial membrane, and also inhibits other glycolysis enzymes – aldolase and phosphofructokinase * *. Clotrimazole in vitro strongly reduces the rate of lactate production by tumor breast tissues (up to 85%), without affecting the production of lactate by normal tissues and the consumption of glucose by both control and tumor tissues *. The results of preclinical studies suggest that the more aggressive the cancer cell, the more effectively clotrimazole acts on it.
Daily subcutaneous injections of clotrimazole (120 mg/kg for 10 weeks) greatly reduced the number of lung metastases in immunodeficient mice *. On a human scale, this dosage is equivalent to about 700 mg/day. The in vitro combination of clotrimazole with imatinib synergistically inhibited the growth of breast cancer cells (T47D) in mice *.
• Vitamin C in very high doses inhibits the glycolytic enzyme GAPDH (the sixth step of glycolysis) and depletes cellular glutathione, leading to energy hunger and oxidative stress*. Intraperitoneal injections of vitamin C (4 g/kg) significantly reduced tumor growth in mice compared to controls *. The human equivalent injection dosage will be approximately 25 g/day. Such overdoses are only acceptable in the short term, for example as an adjunct to radiation or chemotherapy.
• Stiripentol is an antiepileptic drug showed in vitro strong inhibition of glycolysis * and inhibition of the formation of the mammosphere of MCF-7 cells (IC50=100-200 μМ).
• Oroxylin A, a flavonoid from skullcap (Scutellaria baicalensis) root, inhibits in vitro (150 μM) glycolysis in breast carcinoma cells by blocking hexokinase-II (HKII) * *.Wogonin, another flavonoid from skullcap root, inhibits in vitro (2 μM) a lactate dehydrogenase, pyruvate dehydrogenase kinase *, and pyruvate kinase (PK) * in addition to hexokinase.
• Methylglyoxal *, alizarin *, shikonin * inhibit glycolysis in vitro by suppressing other glycolytic enzymes.
The most attractive is the use of hexokinase inhibitors, because it immediately interferes with the production of both energy and building material for creating a daughter cell.
The problem with inhibiting glycolysis is that the glucose taken in by the cell, instead of being spent on energy production, will accumulate inside the cell with all the ensuing negative consequences. To avoid this, such therapy can only be used with a simultaneous reduction in the total caloric content of food consumed.
Suppression of alternative metabolic pathways for energy production. Despite the significant dependence of cancer cells on glycolysis, its suppression has little effect on curbing tumor growth. Limiting glucose intake has its limits, and besides, glucose is not the only source of raw materials for the production of ATP. With an insufficient amount of glucose, cells are able to use alternative, less efficient energy sources, mainly amino acids and lipids. Cells in general show an extraordinary ability to extract energy from available material, including lactic acid *, ketones * and as yet unknown sources *.
Decreased production of ATP from glutamine. Proliferating/glycolytic cells easily switch from glucose to amino acid feedstock, predominantly glutamine.
Glutamine can be used by cells for mitochondrial energy production through oxidative phosphorylation. Just like other sources of energy, glutamine enters the mitochondria, where it participates in a series of closed enzymatic reactions called the Krebs cycle (KC). The molecules formed during this cycle are electron donors for the process of oxidative phosphorylation (OP). During OP, energy is accumulated in the phosphate bonds of the ATP molecule, and then spent on the needs of the cell.
Ideally, from 1 glucose molecule that enters the cell (from 2 pyruvate molecules), you can get energy for 38 ATP units; of these, 8 are in the process of glycolysis (2 directly and 6 indirectly), 6 are in the process of converting pyruvate to acetyl-CoA, and another 24 are in the process of OP. As a final metabolite, 6 molecules of water and 6 molecules of carbon dioxide are formed. Although cancer cells are usually OP disabled due to a poorly functioning electron transport chain, the efficiency of the Krebs cycle enzymes is preserved in them. Therefore, glutamine gets a chance to charge ATP molecules by the so-called substrate phosphorylation in the segment of succinyl-CoA → succinate (FTP) transformations. There is no need for oxygen in this reaction.
Why glutamine and not any other amino acid? First, it is the most abundant amino acid in the body. And secondly, because of the peculiarities of its metabolism. While other amino acids can also provide energy production, glutamine is the only amino acid that does not require energy to be converted metabolically into succinyl-CoA *. Because of this, compared to other amino acids, glutamine provides the highest efficiency in energy production, and for a cancer cell, saving energy is critical.
Thus, cancer cells can obtain a fairly large amount of energy by fermenting glutamine. And, as experiments with glioblastoma cancer cells have shown, they intensively use this opportunity *. Therefore, glucose fasting will be a weakly effective therapy if this alternative energy source is not blocked *.
The strategy of limiting the supply of cells with glutamine may have varying success depending on the subtype of breast cancer. Luminal-type cells are glutamine-independent, while basal-type cells are glutamine-dependent *. Thus, glutaminase inhibitors may be more effective against the most aggressive subtypes, TNBC and HER2+ basal-like breast cancer, but not against ER+ luminal cancer *.
Unfortunately, lowering glutamine levels is more problematic from a practical point of view than lowering glucose levels. Avoiding animal protein and dairy products, as well as plants such as spinach, beans and kale, could help to some extent in solving this problem. However, plant foods contain not only glutamine, but also many other useful nutrients, and its restriction will lead to food inferiority.
In addition, protein and glutamine are also required by normal cells, not just cancer cells. In particular, glutamine is actively used by macrophages, T- and B-cells of the immune system; as well as intestinal cells. In addition, glutamine is required for the transmission of impulses by brain neurons. Therefore, we can only talk about limiting certain foods and changing the structure of the diet in terms of reducing protein intake to a physiological minimum. Since glutamine can be synthesized from other amino acids, and by non-cancerous cells of the tumor itself, it may be worth limiting the intake of any protein during therapy. And perhaps even all these efforts will not be enough if we do not use glutaminolysis inhibitors.
The search for effective and safe inhibitors of glutaminolysis has not yet been very successful, but work in this promising direction does not stop.
• Phenylbutyrate is an aromatic fatty acid that has been clinically tested (300 mg/kg * *) and is used to treat congenital disorders of the urea cycle. Phenylbutyrate metabolites bind to glutamine and excrete it in the urine, significantly reducing plasma levels of phenylbutyrate *.
• Ursolic acid, especially in combination with curcumin or resveratrol, impairs the entry of glutamate into cells *.
• EGCG (epigallocatechin gallate) and other green tea polyphenols * * inhibit some steps in the process of glutaminolysis and lipogenesis, but their efficacy has only been found in preclinical studies, including in mice. The dosage of polyphenols equivalent to a person was 8 mg per 1 kg of body weight, i.e. 500 mg with a body weight of 65 kg.
Production of ATP from lipids. Fatty acids as a fuel for the production of ATP are widely used by cells of the liver, kidneys, muscles, as well as cells of adipose tissue.
In conditions of glucose deficiency, the cells of many other organs and tissues can also resort to lipid metabolism. For example, during prolonged fasting, ketone bodies, which are released into the blood by liver cells during fatty acid metabolism, can be used as fuel molecules. In the end, fat was stored for this, in order to use its energy on a «rainy day».
The accociation between fat intake and cancer risk will be discussed in more detail in the «Diet Therapy» section †. But we must understand that the degree of negative impact of fat on cancer depends on the caloric content of the diet. After all, the cell doesn't care where it gets its energy from, and so total calorie restriction may be more important than the choice of calorie sources.
Although the metabolic pathways for energy production from glucose, amino acids, and fatty acids begin differently, they eventually converge into a common place, the Krebs cycle, and must end in oxidative phosphorylation. Of all the major energy sources (glucose, lipids and amino acids), only glucose is the most efficiently fermentable feedstock. Less effective, but rather competitive, is glutamine. Other energy sources are much less efficient, as they require energy for their metabolism.
A cancer cell can to some extent compensate for a decrease in energy intake in the form of glucose with an energy intake in the form of glutamine. Because both glucose and glutamine are fermentable raw materials. At the same time, ketone bodies (acetoacetate and β-hydroxybutyrate) are not fermentable raw materials. They require oxidative phosphorylation to generate energy. They enter the mitochondria and are included in the Krebs cycle already in the form of succinate, bypassing the metabolic segment of substrate phosphorylation (succinyl-CoA → succinate) *. In addition, the inclusion of ketone bodies in the Krebs cycle can be expected to reduce the cell's use of glutamine because they will compete for the same enzymes in subsequent steps in the Krebs cycle.
But what if we cut off the supply of cells with both glucose and glutamine, and instead of these two sources of energy, supply them with ketone bodies, and in a minimal amount? Then energy production will drop in both normal and cancerous cells. However, normal cells retain the OP mechanism in a sufficiently functional state, which ensures a high ATP yield. Therefore, they can more easily endure an energy crisis by generating energy from ketone bodies. At the same time, cancer cells and other cells with a degraded OP mechanism will be subjected to deadly metabolic stress.
Moreover, in this case, cancer cells will not have to rely on the help of other cells of the tumor microenvironment. Those will not be up to help, they themselves will be in a state of crisis, and compete for the same resources. Therefore, cancer cells will be in a less favorable position in terms of survival and will be forced to stop growing. Cells with the most dysfunctional mitochondria will suffer more than others, and may end their lives in apoptosis.
From such considerations follows the tempting proposal to change the structure of food intake in such a way as to radically reduce the intake of metabolizable carbohydrates and proteins, but increase the intake of fatty acids. Of course, with a minimal reduction in total calorie intake. So-called the ketogenic diet, which will be discussed in more detail below † is based on this theoretical principle. In some clinics, the ketogenic diet is used to a limited extent as an additional therapy, as well as to enhance the therapeutic effect of chemotherapy following this diet.
Dr. Thomas Seyfried * proposed treatment strategy, which he called Press-Pulse, seems reasonable. Here, energy pressure is first applied to the cancer cell (Press). For this, a ketogenic diet is used, in which the overall energy intake is reduced as much as possible. If carbohydrate reduction is used to block glycolysis, then glutaminolysis inhibitors are used to block glutaminolysis. As a result, the enzymatic production of cellular energy drops sharply, severely cutting off the energy supply of the cancer cell *.
Thus, the growth of the cancer cell is suppressed. However, the energy received from the OP may still be enough to keep it alive. Therefore, next step is the impact of chemotherapy (Pulse). In a severe energy crisis, a cancer cell simply does not have the strength to pump toxins out of the cell, and it becomes very vulnerable to chemotherapy. In this way, the dosage of toxins and their negative consequences for the entire body can be reduced. True, such a protocol requires very fine regulation, which is achievable only in a clinical setting.
Decreased production of ATP from aldehydes *. Ketone bodies produced by the liver from fatty acids can be metabolized into aldehydes, and aldehydes can be metabolized by the enzyme aldehyde dihydrogenase (ALDH1) into carboxylic acid. The latter reaction produces NADH, which may be another source of energy for ATP production *.
Suppression of ALDH with gossypol in combination with suppression of mitochondrial complex I with phenformin resulted in depletion of ATP production in cancer cells up to 80%, while normal cells had no loss of ATP production *. This manipulation was accompanied by a reduction in the growth of the grafted tumor in the animals. Gossypol, however, is not a good choice for humans.
Tretinoin (ATRA) in equiv. dose of 0.6 mg/day *
and sulforaphane (sulforaphane) in equiv. at a dose of 320 mg/day *
in animal experiments suppress ALDH, reducing tumor growth, and appear to be more attractive natural inhibitors of ALDH.
Suppression of the production of fuel raw materials inside the tumor. Cancer cells are not the only type of cells that form a tumor. Some of the cells in the tumor microenvironment can convert lactate secreted by glycolytic cells back into pyruvate, which can again be used as fuel by cancer cells. Unfortunately, no way has yet been proposed to avoid this way of feeding cancer cells. Neutralization of lactate in the extracellular space by intratumoral alkaline injections, such as baking soda, looks like an overly adventurous method.
Correction of pyruvate metabolism. Normalization of cellular respiration involves an increase in mitochondrial ATP production, and at the same time suppression of the enzymatic one. While limiting the fuel supply will limit energy production and induce the cell to use it more efficiently, this indirect enforcement will probably not be enough. To force a cell to return to mitochondrial respiration, one has to turn to direct coercion methods.
Inhibition of pyruvate fermentation. Pyruvate is metabolized to lactate by the enzyme lactate dehydrogenase. Neutralization of this biochemical reaction interrupts the metabolic pathway of ATP production characteristic of cancer cells, thereby depriving them of a significant part of their energy.
• Diclofenac * is a non-steroidal anti-inflammatory drug that can affect the transport and release of lactate. Diclofenac has been reported in vitro to reduce tumor growth and lactate levels in the tumor microenvironment * *.
• EGCG (epigallocatechin gallate) * andstiripentol * can also inhibit lactate dehydrogenase to a certain extent.
A double blow to the energy supply of cancer cells (fermentation + weak mitochondria) can bring them to the brink of existence. Therefore, a combination of all the above activities looks more effective.
Activation of the movement of pyruvate into mitochondria. If the fermentation of pyruvate to lactate is blocked, then the pyruvate obtained as a result of glycolysis can be used by mitochondria for oxidative respiration. The problem, however, is not only that the mitochondria themselves do not work well, but that there may be obstacles to the penetration of pyruvate into the mitochondria. For example, the enzyme pyruvate dehydrogenase kinase (PDK) present in the cell inhibits the entry of pyruvate into the mitochondria. There are 4 isotypes of PDK (PDK1-PDK4), and among them, PDK3 has the highest enzymatic activity and is the only enzyme that is not inhibited by high concentrations of pyruvate.
• Sodium dichloroacetate (DCA) * * is an analogue of acetic acid in which two of the three hydrogen atoms of the methyl group are replaced by chlorine atoms (CHCl2COOH). DCA salts inhibit PDK *, which increases pyruvate influx, providing mitochondria with raw materials for oxidative respiration. And the activation of oxidative metabolism in breast cancer, in turn, leads to a decrease in metastasis and a decrease in tumor growth *. Unfortunately, DCA inhibits different isotypes of PDK with varying strengths, and PDK3 appears to be the most stable of them *.
DCA has been clinically tested for the treatment of lactic acidosis *. In patients with head and neck squamous cell carcinoma, complete response rates at the end of treatment were significantly higher in the DCA group compared with placebo (71% vs. 38%). However, survival results did not differ significantly between groups *.
DCA therapy is complicated by its limited ability to reach target mitochondria *. However, the addition of coenzyme Q10, acetyl-L-carnitine, B complex, magnesium, and lipoic acid help enhance its therapeutic effect *.
Dosage of sodium dichloroacetate: (1'000-3'500 mg/day *), usually started at 15 mg/kg body weight. The dichloroacetate salt is diluted in 100 ml of water and taken 2-4 times a day. With a deterioration in well-being, the reception is stopped. Since DCA is a pyruvate mimetic, it can be used for a long time without fear of becoming addictive. Although DCA has been a proven drug for decades to treat children with congenital disorders of mitochondrial metabolism, it is not recommended for prophylactic use.
The figure presented here shows all the efforts proposed above to correct the metabolism of a cancer cell in order to put it before a choice: switch to mitochondrial respiration or die.
If mitochondrial DNA mutations prevent a cell from fully utilizing OP, it will be difficult for it to survive. It cannot be said, however, that this method will be sufficiently successful.
Firstly, a general (instead of local) effect on cells will depress the energy of all other cells in the body, not just cancer cells. This, of course, can heal the body as a whole, rejecting cells with poorly functioning mitochondria and keeping regenerating cells from the final transition to glycolysis. However, there are many normal cells in the body that use only glycolytic ATP production. Strong inhibition of glycolysis will affect the work of cells such as red blood cells or retinal cells. Whereas we should only target cancer cells.
Secondly, the delivery of therapeutic substances into the tumor in a natural way is difficult. And their introduction directly into the tumor is not always possible. But even if this problem is solved, we return to the first point: the tumor does not consist only of cancer cells. We cannot selectively deliver active substances to our target – cancer cells, they will also come to normal cells that form tumors. For example, immune cells. And we cannot predict how their functionality will change from our actions.
Thus, manipulation of the metabolism of tumor cells has its definite limit. Nevertheless, it can make a significant contribution to the antitumor fight, being included in the complex therapy.
All attempts to increase the oxygen respiration of tumor cells may be unsuccessful if the main participant in this process, oxygen, is deficient.
Low oxygen concentration is a key factor in the high acidity in the tumor and the activity of the tumor process. Lack of oxygen enhances glycolysis in cells and causes malignant transformation of their phenotype (Warburg effect). Conversely, the presence of oxygen causes the suppression of glycolysis (Pasteur effect).
Increasing oxygen concentration in tissue. Tumor hypoxia poses a serious obstacle to effective cancer therapy *. For example, the main mechanism of radiation therapy is the creation of a high concentration of reactive oxygen species; therefore, oxygen deficiency gives hypoxic tumors a much higher radiation resistance. Many chemotherapy drugs also lose their therapeutic efficacy under hypoxic conditions. Finally, hypoxia reduces the effectiveness of immunotherapy. Thus, an increase in oxygen concentration due to a decrease in acidity in the tumor microenvironment and an increase in oxygen delivery to the tumor are extremely important factors in antitumor therapy.
Decreased acidity in tissues will be discussed separately in the «Acid-Alkaline Balance» section †. And the concentration of oxygen in the blood can be increased in several ways:
- With the help of natural carriers (erythrocytes). Lack of oxygen can be caused by both low red blood cells and a lack of hemoglobin, which reduces the ability of red blood cells to carry oxygen. The latter can be caused by a deficiency in the diet of chemical elements (zinc, iron) and nutrients (vitamin B12, folate), poor absorption, kidney failure, blood loss and other reasons.
- With the help of synthetic carriers. In addition to red blood cells, alternative oxygen carriers in the blood can be used, but they still remain difficult to access.
- By increasing blood flow. Increasing blood circulation, for example by vasodilation, improves its ability to deliver oxygen *, minerals and nutrients, and also improves the effectiveness of both therapeutic agents and the prevention of metastasis. To do this, you can use both physiotherapy and some supplements, for example, vasodilators. Deterioration of blood circulation can be caused by high aggregation of red blood cells and microthrombosis, which may require additional efforts.
- By directly dissolving oxygen in the blood. Increasing the oxygen concentration in the blood directly, bypassing the carriers, can be done by inhaling a gas with a very high oxygen content – both at normal atmospheric pressure and at elevated pressure (hyperbaric oxygenation). The latter requires special equipment and the services of qualified personnel.
The last point needs further clarification. Prolonged breathing with pure oxygen can bring not only benefits, but also harm. First, oxygen without the addition of carbon dioxide causes blood vessels to constrict. Thus, it is possible not only not to increase, but, on the contrary, to weaken the delivery of oxygen. Secondly, oxygen is prone to the formation of reactive oxygen species (ROS), which have a destructive effect on any proteins in our body.
It is also worth remembering that prolonged exposure to vasodilators increases the supply of not only oxygen, but also energy sources – glucose and glutamine. If glycolysis and glutaminolysis are not suppressed at the same time as increased blood circulation, this can contribute to the advancement of cancer, which again emphasizes the need for a comprehensive approach to cancer treatment.
Local hyperthermia (41-42 °С) enhances the movement of fluid in the tumor and weakens the resistance of cancer cells to radiation therapy *. Hyperthermia may improve oxygenation of hypoxic breast tumors *. The effect of hyperthermia can last for a day after the session *.
Although the combination of hyperthermia and standard treatment may enhance the therapeutic effect, there is no consensus regarding the use of hyperthermia outside the course of treatment due to the lack of knowledge of this topic. There is a danger that increased circulation of fluid may contribute to the spread of tumor cells. A similar risk applies to massage, infrared and ultrasonic irradiation of the tumor zone. Thus, hyperthermia can only be considered as a therapy in combination with other therapies.
Proteolytic enzymes are enzymes that help break down protein. Their activity is regulated in such a way that they destroy foreign, dead or non-functional protein structures without affecting the functional cells of the body.
Proteolytic enzymes improve blood flow by cleaning the walls of blood vessels and reducing the level of fibrinogen *, which also reduces blood pressure *. They cleanse both the blood itself and the cells contained in it from fibrin and mucus, and thereby expose antigens on the surface of cancer cells to the immune system, reducing the risk of metastasis. Of the entire set of proteolytic enzymes, only a few have been sufficiently studied.
Trypsin and chymotrypsin are the most effective *,
but they are difficult to obtain.
Bromelain and papain are extracted, respectively, from pineapple stem and papaya fruit; and their prices are more reasonable.
Serrapeptase (3×10 mg) has long been used in sports medicine to reduce inflammation in injuries and sprains. Among all the proteolytic enzymes on the market, serrapeptase seems to be the most profitable offer.
Nattokinase (2×1'000-1'440 fibrinolytic units) has become another popular thrombolytic enzyme in recent years, but its price is not yet attractive.
Lumbrokinase contains a group of proteolytic enzymes, including plasminogen activator and plasmin. It is obtained from the reddish puffball earthworm (Lumbricus rubellus). According to its fibrinolytic properties, lumbrokinase is 30 times stronger than nattokinase and 300 times stronger than serrapeptase, but its price is too high.
Different enzymes are most active at different levels of acidity, and therefore a complex containing trypsin, chymotrypsin, bromelain, papain, serrapeptase will apparently be more versatile than any of these enzymes alone. An example of such a complex is Wobenzim™. Dosage: 600-1'000 mg/day, but not more than 4'000 mg/day *. Long-term use without interruption is allowed, but caution should be exercised. The combination of proteolytic enzymes and their high dosage enhances the effect of other anticoagulants, which in many cases can be very dangerous.
NSAIDs are non-steroidal anti-inflammatory drugs.
• Acetylsalicylic acid counteracts DNA mutation, reducing the risk of any form of cancer. In addition, it prevents platelet aggregation – aggregation, thereby improving blood flow. Because platelets shield circulating cancer cells from detection and destruction by immune cells, and make it easier for them to attach to epithelial walls at distant sites, aspirin is able to counteract metastasis. Aspirin also reduces the thrombogenic effect of some therapeutic agents, such as tamoxifen. The combination of ginkgo extract (450 mg/day) with aspirin (100 mg/day) enhanced their antiplatelet effect in post-stroke patients in a clinical trial *. Dosage: 100 mg/day.
Long-term use of aspirin, although possible, is undesirable due to possible damage to the epithelium of the gastrointestinal tract and increased intestinal permeability. Fortunately, salicylates are found in high concentrations not only in willow bark, but also in many foods *. Examples are mint, cumin, thyme, paprika, turmeric, kalinji, cardamom *. Their widespread use as a condiment would reduce the dosage of aspirin itself.
• Naizilat® (amtolmetin guacil). A modern non-steroidal anti-inflammatory drug, an attractive alternative to aspirin. Reduces thrombosis, improves blood flow. Dosage: 600 mg/day. It is taken on an empty stomach.
Another aspect of the antitumor activity of NSAIDs, such as celecoxib, is the ability to directly inhibit mitochondrial respiration, transmembrane electrical potential and ATP production, causing an excess of ROS, triggering apoptosis of cancer cells, and also reducing the ability of cancer cells to migrate * *.
Dibazol is a well-known vasodilator. Dibazol relaxes the muscles of the walls of blood vessels, improving blood circulation. In addition, it acts as a weak immune system stimulant. Unlike acetylsalicylic acid, dibazol does not cause acidification of body tissues. Dosage: 3×20 mg 2 hours before or 2 hours after meals.
Vitamin B3 (vitamin PP, niacin, nicotinic acid, nicotinamide) expands small blood vessels (including the brain), improving blood microcirculation. It has a weak anticoagulant effect, normalizes blood cholesterol, and also has detoxification properties. The dosage for healthy people is 20 mg/day. Overdose up to 100 mg/day is not harmful.
Arginine (3×700 mg) is an essential acid capable of producing nitric oxide (NO), which causes smooth muscle cells to relax. As a result, blood vessels dilate, increasing blood flow and improving oxygen delivery to tissues.
Flax-seed. In mice, the consumption of ground flaxseed (10% of the total diet) during tamoxifen therapy resulted in a decrease in the density of microvessels in the tumor and a decrease in the release of the pro-inflammatory cytokine IL-1 *. The combination of flaxseed and tamoxifen inhibited grafted tumor size by more than 53% in mice compared to tamoxifen alone *.
Some plants improve blood circulation in small vessels and capillaries.
• Horse chestnut (Aesculus hippocastanum) contains aescin, which reduces inflammation and reduces congestion in veins and small vessels * by reducing capillary permeability. In addition to escin, the horse chestnut fruits contain p-coumaric acid, caffeic acid, quercetin, kaempferol and apigenin. Water-alcohol extract of fruits: 250-300 mg 2 times a day *, i.e. 100-150 mg of escin per day * *.
• Ginkgo biloba (Ginkgo biloba) contains flavonoids and terpenoids, which help to increase the tone of arterial and capillary vessels, and favor the improvement of cognitive ability *. In addition, ginkgo extract protects mitochondrial DNA from oxidative damage *, and improves mitochondrial respiration *. Leaf extract: 40-120 mg 2 times a day *.
• Centella (Centella asiatica), aka Gotu Kola. Reduces platelet aggregation and improves blood circulation, including in the brain, promotes relaxation, relieves anxiety symptoms * and improves cognitive ability *. Dried leaf extract: 60 mg 1-2 times a day. It is not recommended to take the plant for more than 6 weeks in a row.
• Sage (Salvia miltiorrhiza) contains polyphenols and tanshinones, which in vivo prevent platelet aggregation, thus improving blood flow * *.
• Hawthorn (Crataegus) contains procyanidins and flavonoids that dilate blood vessels, prevent thrombosis and reduce capillary permeability *. Hawthorn extract: 160-900 mg two to three times a day, which corresponds to 30-170 mg of procyanidins and 3.5-20 mg of flavonoids.
Each of these funds can be taken in turn, alternating every 1.5-3 months.
Known platelet inhibitors are inositol, ginseng, turmeric, ginger, flaxseed oil, fish oil, vitamin E. Caution should be exercised in their use, however, because excessive inhibition of platelets can cause internal bleeding as well as internal bleeding. Reception of the funds discussed above should be stopped starting 2 weeks before the operation, and resumed no earlier than 1 week after the operation, in agreement with the doctor.
Considering that the above means enhance the effect of each other, when they are taken together, the dosage should be significantly reduced.
Reducing oxygen demand. An alternative and perhaps more effective solution to the problem of hypoxia is not to satisfy the cellular demand for oxygen, but to reduce this demand. Reducing oxygen consumption by cells reduces its depletion in the tissue, thereby increasing oxygen saturation. Computer simulations show that a 30% reduction in oxygen consumption is as effective at reversing hypoxia as a 4-fold increase in blood flow *. For this, the following means can be used:
• Atovaquone is an antimalarial drug that in vitro reduces tumor hypoxia and enhances the effect of radiation therapy *.
• Sodium hydrosulfide (NaHS) is a donor that releases hydrogen sulfide (H2S). NaHS interferes with the respiratory chain of the mitochondria of tumor cells, improves the oxygen saturation of tumors and increases the effectiveness of radiation therapy. Tumors irradiated 15 minutes after a single injection of NaHS were twice as sensitive to radiation therapy as tumors that received radiation alone *. NaHS is not used clinically.
• NSAIDs (Non-Steroidal Anti-Inflammatory Drugs) such as diclofenac, indomethacin, and piroxicam reduce hypoxia in liver tumors and fibrosarcomas in mice within half an hour *.
• Metformin is an antidiabetic drug. Metformin treatment (equiv. 1'000 mg/day) significantly improved the oxygenation of the grafted tumor in mice *. This dosage does not exceed that used in the treatment of diabetes in humans.
It is important to understand that in addition to the forced increase in the oxygen level in the tumor, many physiological factors also influence the oxygen level in the tumor tissue. Thyroid hormones, for example, play a major role in metabolic activity and oxygen uptake by cells. Higher levels of the T4 hormone are associated with a higher risk of any type of cancer, including breast cancer *. Thus, the health of the thyroid gland strongly affects the oxygen saturation of the tissue and the effectiveness of antitumor therapy.